Prostate Cancer Treatment Paradox
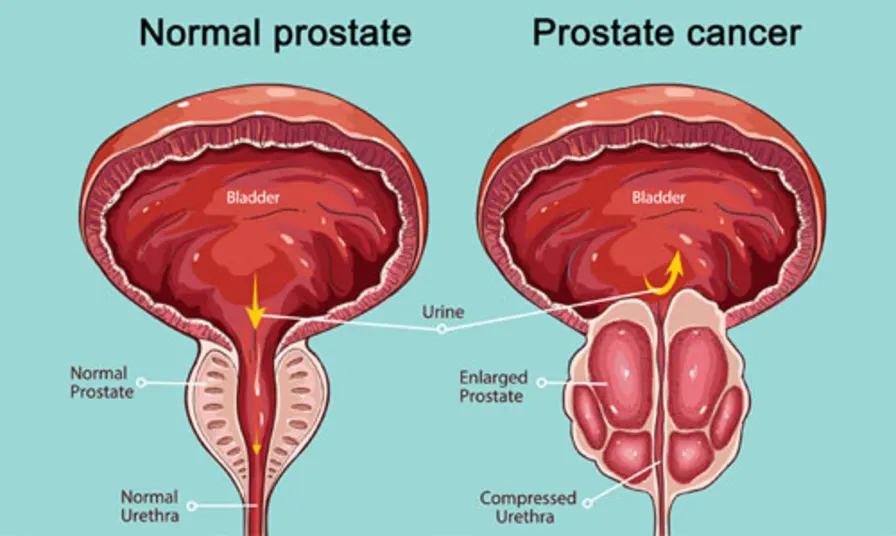
Prostate Cancer
The treatment of prostate cancer presents a notable paradox, particularly concerning the role of testosterone. Recent research highlights how testosterone, typically viewed as a growth factor for prostate cancer, can also inhibit tumor growth under certain conditions. This blog will explore the complexities of this phenomenon, known as the testosterone paradox, and its implications for treatment strategies.
Understanding the Testosterone Paradox
Historically, testosterone suppression has been a cornerstone of prostate cancer treatment, especially in early-stage disease. Blocking testosterone production has proven effective in halting tumor growth. However, emerging evidence suggests that in advanced stages of prostate cancer, elevating testosterone levels may actually delay disease progression. This duality poses significant challenges for clinicians and researchers alike.
Mechanisms Behind the Paradox
- Hormonal Influence on Cancer Cells: Research indicates that prostate cancer cells are equipped to respond differently to varying testosterone levels. At low testosterone levels, cancer cells tend to proliferate. Conversely, when testosterone levels are elevated, these cells undergo differentiation, which suppresses tumor growth. This mechanism is facilitated by the androgen receptor, which behaves differently depending on the hormone concentration—acting independently at low levels and forming dimers at higher levels to inhibit growth.
- Bi-Polar Androgen Therapy (BAT): This innovative treatment approach involves administering high doses of testosterone to patients with advanced prostate cancer. Studies have shown that BAT can lead to paradoxical growth inhibition of tumors, suggesting that supraphysiological levels of testosterone may activate immune pathways and induce cell death mechanisms that are beneficial in the context of advanced disease.
Clinical Implications
The paradox of testosterone in prostate cancer treatment raises several clinical considerations:
- Treatment Timing and Strategy: The timing of when to initiate testosterone suppression versus elevation is crucial. For early-stage disease, suppression remains the standard; however, for advanced cases, BAT may offer a new therapeutic avenue.
- Personalized Medicine: Given the biological variability among patients, understanding individual responses to testosterone levels can help tailor treatment plans. This personalization is vital in optimizing outcomes and minimizing unnecessary treatments.
- Research and Development: Ongoing studies are essential to fully elucidate the mechanisms behind the testosterone paradox. Researchers are working on developing new drugs that exploit this knowledge, potentially leading to more effective therapies for advanced prostate cancer patients.
Recent Findings and Future Directions
Recent studies, including those led by the Duke Cancer Institute, have provided critical insights into the testosterone paradox. These findings underline the necessity for further research to define optimal treatment protocols and explore the potential of BAT as a standard practice for specific patient populations.
Conclusion
The treatment paradox surrounding testosterone in prostate cancer illustrates the complexity of hormonal influences on cancer biology. As research progresses, it is hoped that a clearer understanding of these mechanisms will lead to improved therapeutic strategies, ultimately enhancing patient outcomes in this challenging disease landscape. The dual role of testosterone underscores the need for a nuanced approach to prostate cancer treatment, balancing the benefits of hormone suppression with the potential advantages of elevation in advanced cases.In summary, the testosterone paradox not only challenges existing treatment paradigms but also opens new avenues for research and clinical practice, paving the way for more effective and personalized prostate cancer therapies.






